Low Level Laser Therapy
Low‑Level Laser Therapy (LLLT) is a safe, non-invasive treatment that uses specific wavelengths of light to reduce pain, calm inflammation, and support the body’s natural healing processes. It’s completely painless and drug-free – making it a great option for managing a wide range of foot and lower limb conditions.
LLLT works by delivering targeted light energy into the body’s tissues, where it is absorbed at a cellular level. It promotes the production of energy within the cells, encouraging faster healing while also calming overactive nerves that contribute to pain.
The targeted light absorbed by cells helps to:
- Increase blood flow and oxygen to the area
- Reduce inflammation by clearing waste products and swelling
- Stimulate cell repair and collagen production
- Block pain signals by calming overactive nerves
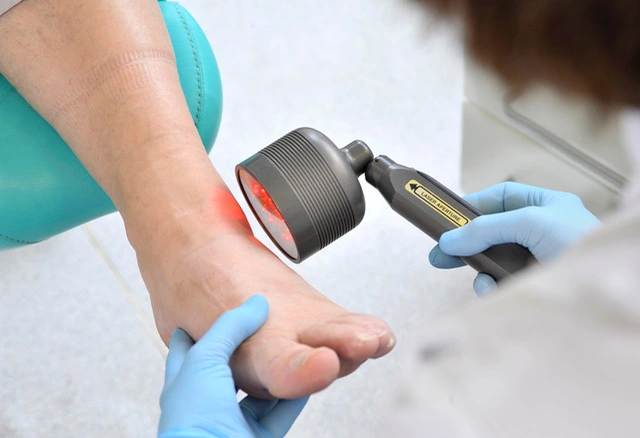
What To Expect
Treatment sessions are quick and comfortable, typically lasting 10 – 25 minutes, depending on the condition being treated. Most patients feel nothing at all during the session, or just a gentle warmth. A course of treatment usually involves 6 to 12 sessions, spaced over several weeks, and can be used alone or alongside other therapies such as orthotics or exercise plans.
Conditions Treated with Low-Level Laser Therapy
Low-Level Laser Therapy can be used for a wide range of foot and lower limb conditions, including:
- Gout
- Fungal Toe Nails (Onychauxis)
- Achilles Tendon Rupture
- Bursitis
- Haglund’s Bump
- Morton’s Neuroma
- Plantar Fasciitis
- Sever’s Disease
- Achilles Tendinitis